3 March 2014
399 view(s)
Endometriosis Awareness Week - Let's Beat the Invisible Disease
Endometriosis affects 1.5million women in the UK. Despite being so common, it is not a well-known condition. Despite being an incredibly serious, painful and debilitating condition, endometriosis is often referred as an ‘invisible disease’ as the symptoms are not outwardly obvious to the untrained eye.
This can make it harder for women to get the help and support they need, not only from doctors but from family, friends and colleagues who are unaware of just how difficult living with endometriosis is.
 March is International Endometriosis Awareness Month and an opportunity to raise the profile of the condition. For many women it can take months or even years to get a diagnosis, and this is partly due to both themselves and their doctor not being familiar with the condition.
The more people know about the condition, the more they can offer support to those who suffer from it and help to campaign for more research. By researching endometriosis we can help to find more effective and long term treatments to reduce the suffering of those affected by it.
March is International Endometriosis Awareness Month and an opportunity to raise the profile of the condition. For many women it can take months or even years to get a diagnosis, and this is partly due to both themselves and their doctor not being familiar with the condition.
The more people know about the condition, the more they can offer support to those who suffer from it and help to campaign for more research. By researching endometriosis we can help to find more effective and long term treatments to reduce the suffering of those affected by it.

 You may find that yoga, pilates and other gentle, low intensity exercise methods are helpful as they will allow you to strengthen your core and improve flexibility which could help to prevent fibrous internal scar tissue forming. Yoga Tune Up Coregeous is a brilliant gentle workout to strengthen your entire core, whilst Pfilates and Katy Bowman's Down There for Women are both geared towards pelvic health.
You may find that yoga, pilates and other gentle, low intensity exercise methods are helpful as they will allow you to strengthen your core and improve flexibility which could help to prevent fibrous internal scar tissue forming. Yoga Tune Up Coregeous is a brilliant gentle workout to strengthen your entire core, whilst Pfilates and Katy Bowman's Down There for Women are both geared towards pelvic health.
 March is International Endometriosis Awareness Month and an opportunity to raise the profile of the condition. For many women it can take months or even years to get a diagnosis, and this is partly due to both themselves and their doctor not being familiar with the condition.
The more people know about the condition, the more they can offer support to those who suffer from it and help to campaign for more research. By researching endometriosis we can help to find more effective and long term treatments to reduce the suffering of those affected by it.
March is International Endometriosis Awareness Month and an opportunity to raise the profile of the condition. For many women it can take months or even years to get a diagnosis, and this is partly due to both themselves and their doctor not being familiar with the condition.
The more people know about the condition, the more they can offer support to those who suffer from it and help to campaign for more research. By researching endometriosis we can help to find more effective and long term treatments to reduce the suffering of those affected by it.
What is Endometriosis?
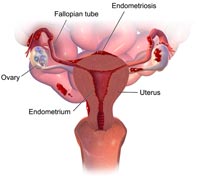
Endometriosis occurs when cells like those on the lining of the womb (endometrial cells) occur elsewhere inside the body. Usually it is around the pelvic area on the outside of the uterus, fallopian tubes and ovaries, but can also occur on the rectum, bowel, and bladder. In rare instances it can occur on the skin, eyes, spine, lungs and even the brain. Every month as a result of hormone changes the lining of the womb breaks down and bleeds in preparation for a fertilized egg – this is our period. For women with endometriosis, this also causes bleeding outside the womb in whichever area the endometrial cells have grown. Period cramps can be painful enough anyway, but imagine having to deal with that pain elsewhere in your body too, each time you have a period. On top of this, bear in mind that the internal bleeding has no way of leaving the body like normal menstrual blood can. This can lead to severe inflammation, internal scarring and growth of blood-filled cysts which can eventually burst and cause even more severe pain. For some women internal scarring can be so severe that adhesions form between organs. These fibrous bands of scar tissue can fuse organs together, causing constant chronic pain and pelvic floor dysfunction. The pelvic organs – the uterus, bladder, rectum and lower intestines – are all supported by the pelvic floor, so if adhesions cause the organs to fuse this has a knock-on effect on pelvic floor strength and can lead to bladder and bowel weakness, plus persistent pelvic pain.
What causes endometriosis?
There are several theories, but not one which explains the exact cause of endometriosis. That’s why more research needs to be done on the condition; knowing the cause could help with developing treatments. Just a few theories include:- Retrograde menstruation – the theory that menstrual fluid flows backwards through the fallopian tubes and into the abdomen where endometrial cells then grow.
- Circulatory and/or lymphatic spread – the theory that endometrial tissue particles travel through the body via the bloodstream or lymphatic system.
- Genetics – the theory that endometriosis runs in the family and is passed down through generations via our genes.
- Environmental factors – the theory that toxins in the environment cause endometriosis or affect our immune system to make us more susceptible to it.
- Immune dysfunction – the theory that women with endometriosis have a weaker immune system and therefore cannot fight off the condition.
- Metaplasia – the theory that normal cells morph into endometrial cells, usually as a result of inflammation which causes the cells to adapt to a different environment.
What are the symptoms of endometriosis?
There are lots of classic endometriosis symptoms to look out for, but the trouble is that many of them can occur as a result of other conditions, which can make endometriosis difficult to diagnose.Symptoms include:
- Severely painful periods
- Back and/or leg pain
- Pain during sex and/or after sex
- Difficulty getting pregnant
- Period pain when your period is not due
- Spotting in between periods
- Particularly long periods
- Irregular periods
- Unusually dark blood during your period
- Blood in your urine or stools
- Pain when urinating
- Painful bowel movements
- Irritable bowel symptoms e.g. diarrhoea, constipation and abdominal pain
- Prone to infections such as thrush and BV
- Lethargy
- Nausea
- Depression
- Feeling faint and/or dizzy
I think I have endometriosis – what should I do?
Visit your doctor as soon as you can, who will be able to examine you and send you for further tests. The only definitive test for endometriosis that can confirm you have the condition is called a laparoscopy. This is when a small camera is inserted into the pelvic area via a keyhole incision in the abdomen. The procedure requires a general anaesthetic but since the incision for the camera is so small recovery time is fast and there is very little risk of complications. If you’ve been trying for a baby and have had difficulty getting pregnant, it could be a sign of endometriosis and it’s a good idea to visit your doctor. In some instances women do not have any symptoms of endometriosis other than infertility, so it is definitely worth visiting your GP and being checked for endometriosis.How is endometriosis treated?
There is no definitive cure for endometriosis, but there are a number of treatment options available, from treating the pain and inflammation to removing the endometrial cells themselves.Pain relief medication
Anti-inflammatory pain relief drugs such as ibuprofen are preferred as they help to reduce swelling caused by the condition. You can take them for a few days before your period is due to prevent the inflammation. Codeine may be helpful for severe pain, but it can cause constipation which often aggravates the symptoms of endometriosis. Plus, it can make you drowsy and nauseous which means it may not be very practical to take during the day when at work or out and about.Hormone treatments
Since endometriosis flares up during your period with changing hormone levels, for many women hormone treatments are a good solution to alleviate their symptoms. Sometimes the contraceptive pill can help, but some women require more intensive hormone treatments which come with their own side effects. Nausea, headaches, dizziness, high blood pressure and depression are all potential side effects, and may be even more difficult to deal with than the symptoms of endometriosis. Just like with the contraceptive pill, it may be a case of trying a few different types of hormone treatments before you find the one that works best for you.Laparoscopic surgery
This is a key-hole procedure in which a small incision is made into your abdomen to allow the removal of endometrial tissue. This is performed under general anaesthetic and since the incision is small recovery is relatively quick. The downside is that it isn’t suitable for women with extensive endometrial tissue, and there is a risk that the endometriosis could come back if some tissue is left behind.Laparotomy
This is similar to the procedure above, but is for women who have extensive endometrial tissue or in cases where organs have fused together as a result of the tissue growth. It involves a cut right across the bikini line to give the surgeon better access than they would have during keyhole surgery. Since the incision is much larger, recovery is a slower process and you could be left with scarring.Hysterectomy
This is often treated as a last resort for women with severe endometriosis who have tried all other options. Hysterectomy is the removal of the womb, and has a significant impact on your body. Firstly, you will not be able to have children. Secondly, your body may go through the menopause earlier than normal which comes with its own set of symptoms and side effects. Sometimes HRT is prescribed to alleviate the early menopause, but this can actually cause the endometriosis to return, particularly if some endometrial tissue was left behind. Not only this, but HRT can also cause nasty side effects such as nausea, dizziness, headaches and high blood pressure. An alternative to a full hysterectomy is to remove the uterus but to leave the ovaries which will stop the onset of menopause. However in this case it is even more likely that the endometriosis will return and cause the same severity of symptoms as before the hysterectomy. For some women having a hysterectomy provides complete relief from the symptoms of endometriosis, but it is a major procedure and requires a lot of consideration to decide if it is the best option for you. Your GP or specialist will be able to talk through the pros and cons with you to help you come to a decision.
Will endometriosis stop me from having children?
Endometriosis can make it difficult to conceive but it depends on the severity of your endometriosis, the location of the endometrial cells and the type of treatment you opt for. Your doctor or specialist will be able to give you more advice on the best treatments option to help you get pregnant. Destroying or removing the endometrial tissue (laparoscopy or laparotomy) is often a good option for women who want to conceive. Although the tissue could eventually come back, it could provide you with an endometriosis-free window during which time your chances of conceiving will be significantly improved. The symptoms of endometriosis tend to dissipate during pregnancy. This is because you no longer have periods, which prevents the painful bleeding of endometrial cells. However, it is a myth that having children cures endometriosis; there is a good chance the condition will return after pregnancy when your menstrual cycle returns.What can I do to manage my endometriosis?
If you choose not to have surgery to treat your endometriosis, or if you still suffer from it despite having surgery, there are several ways that you can manage your condition and control your pain.Change your diet
It’s amazing the impact food can have on our body without us really realising it, and changing your diet may be a good way to help manage your endometriosis symptoms. Certain food types such as wheat, sugar and saturated fats can stimulate inflammation or bloating and should be avoided. Others can help to regulate hormone production to ease your symptoms, such as broccoli, cabbage and dark green veggies. With a little research you can easily find a list of foods to avoid or eat more of based on your personal symptoms.Use a Squatty Potty
Endometriosis can cause symptoms like IBS – diarrhoea, constipation and bloating – which in itself is uncomfortable, but more so if you’re suffering from severe period cramps too. Squatty Potty puts your body in a more natural position when on the loo, making bowel movements easier and more complete. This will help to prevent constipation, reduce bloating and could relieve a little pain too.Switch to menstrual cups
Menstrual cups can hold up to 3 times more fluid than disposable products, so if your periods are particularly heavy as a result of endometriosis you may find a cup is more convenient. Many women also report that menstrual cups reduce period pain. The theory is that cups are worn lower down in the vagina and therefore allow menstrual fluid and larger blood clots to flow more naturally rather than remaining backed up inside the body causing further pain.Try TENS machines
Although some women may be able to manage their endometriosis pain with over-the-counter drugs such as paracetamol and ibuprofen, others will need to be prescribed more powerful medication to cope. Strong pain relief meds can cause drowsiness and nausea which isn’t practical when you’re at work or and out and about and need to be alert. TENS could be a good solution. It delivers mild electrical stimulation to the nerves via electrode pads to block pain signals. Try attaching the electrodes to your lower abdomen or back, or wherever you’re feeling pain (for some it’s in the legs). Not only will TENS give you almost immediate relief from pain, the effects can last for a couple of hours. Try the OVA which is designed for period pain, or the Beurer EM10 Mini Pad which is small, discreet and completely portable.Do pelvic floor exercises
Internal scarring and adhesions caused by internal bleeding can cause chronic pain and pelvic floor weakness. By doing your pelvic floor exercises you can help to keep your muscles nice and strong as well as relieve pain. Head over to www.kegel8.co.uk for some brilliant guides on how to do your pelvic floor exercises, or alternatively you could try EMS - electronic muscle stimulation. If you’re looking for an EMS pelvic floor exerciser we highly recommend the Kegel8 Ultra 20 which has 3 clinically-designed programmes for pelvic pain, plus a collection of programmes designed for strengthening the pelvic floor. EMS works in a similar way to a TENS machine – mild electrical currents stimulate the nerves – except it contracts and relaxes the muscles rather than just blocking pain signals. Not only does this strengthen the muscles, it also helps to relax tight muscles and increase circulation throughout the muscles to relieve pain. Kegel8 Ultra 20 can be used with a vaginal probe, or if that is too painful, it can be used with surface skin electrodes on the abdomen or back to relieve pain.Take supplements
Since endometriosis is linked with low immunity it’s a good idea to take some good quality supplements to make sure your vitamin and mineral levels are healthy. This may not directly relieve your symptoms, but it will help the rest of your body to stay healthy whilst battling the endometriosis which could help to stop you feeling so lethargic and dizzy.Exercise
As long as you don’t overdo it, exercise could help to reduce your pain. This is because it releases endorphins which help to block pain signals and improve your mood. Take it steady to begin with; a brisk walk or gentle jog will probably be enough to get your blood pumping without tiring you out. If you at any time feel dizzy or your symptoms get worse as a result of exercise you should see your doctor. You may find that yoga, pilates and other gentle, low intensity exercise methods are helpful as they will allow you to strengthen your core and improve flexibility which could help to prevent fibrous internal scar tissue forming. Yoga Tune Up Coregeous is a brilliant gentle workout to strengthen your entire core, whilst Pfilates and Katy Bowman's Down There for Women are both geared towards pelvic health.
You may find that yoga, pilates and other gentle, low intensity exercise methods are helpful as they will allow you to strengthen your core and improve flexibility which could help to prevent fibrous internal scar tissue forming. Yoga Tune Up Coregeous is a brilliant gentle workout to strengthen your entire core, whilst Pfilates and Katy Bowman's Down There for Women are both geared towards pelvic health.